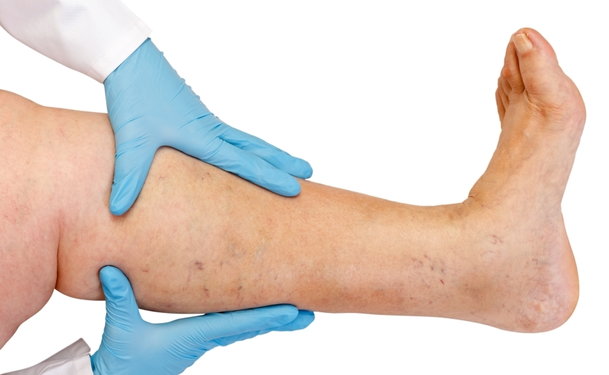
Venous ulcers are the most common type of ulcers occurring in the lower limbs, accounting for more than half of all ulcer cases. A venous ulcer typically appears as a wound or skin ulcer, resulting from a breakdown of the surrounding cells and tissue layers.
Causes of Venous Leg Ulcers
Venous leg ulcers occur when the one-way valves of the veins fail to maintain the blood flow toward the heart and prevent any back flow. This problem with blood flow is known as venous insufficiency. The venous system in the lower limbs includes the deep, superficial and profound veins; where the deep veins lie between the muscles, the superficial veins in the upper layers just below the skin, and the profound veins are located in between, connecting the other two types of veins. In damaged valves, the blood backs up and pools in the veins, building up pressure, which prevents nutrients and oxygen in the blood from reaching the body tissue. Eventually, the tissue breaks down and forms an ulcer.
Signs and Symptoms of Venous Leg Ulcers
Lower limbs are the most common sites of venous ulcers, especially the inner areas of the ankle and legs. A sign of potential trouble can be detected when the skin starts turning a brown-purple color (indicating blood pooling in veins) and the legs swell. While the ulcer itself is usually painless, the surrounding tissue might get dry, itchy and thickened, or it might get infected; in which case, it will emit a foul odor and pus may drain out of it.
Risk Factors
Venous ulcers are much more likely to occur in:
- Elderly people (the risk increases with age)
- People who stand for long periods or on a daily basis, as with certain jobs
- Cases of previous vein inflammation (phlebitis) or obstruction (deep vein thrombosis)
- Bedridden patients or long-distance travelers who do not move for long periods
- Pregnancy (the risk increases with multiple pregnancies)
- Obesity, smoking and excessive alcohol consumption
- Patients with chronic medical illnesses, such as diabetes mellitus, high cholesterol and others that affect the body's immune system and capacity to heal
Treatment Options for Venous Leg Ulcers
Treating a venous ulcer is based on the status of circulation. Better circulation leads to easier treatment, better healing and fewer complications. Treatment can include raising the legs above the heart level as often as possible and wearing compression socks. These measures can improve circulation and prevent blood from pooling in the veins. Regular walking and exercising are also recommended to help improve circulation and encourage healing. Another important medical intervention is to treat the underlying cause of a venous ulcer, which may include improving the management and control of any chronic illnesses that are present.
Sometimes extensive wound cleansing is needed. Antibiotics can be given orally or applied directly on the ulcer, along with a wet dressing or drying agents, as appropriate. In some cases, a graft (skin taken from other parts of body) is used to cover the ulcer to heal it.
Prevention of Venous Leg Ulcers
To help prevent venous leg ulcers, these measures may be followed:
- Avoid long periods of standing or sitting
- Raise the legs above the heart and use compression socks as often as possible
- Maintain a healthy lifestyle that includes regular moderate exercise, a healthy diet (low in fat, rich in fruits and vegetables) and reduce body weight, if overweight
- Quit smoking, reduce alcohol consumption and try to stay active
- Inspect the lower limbs daily and look for any color changes or cracks in the skin