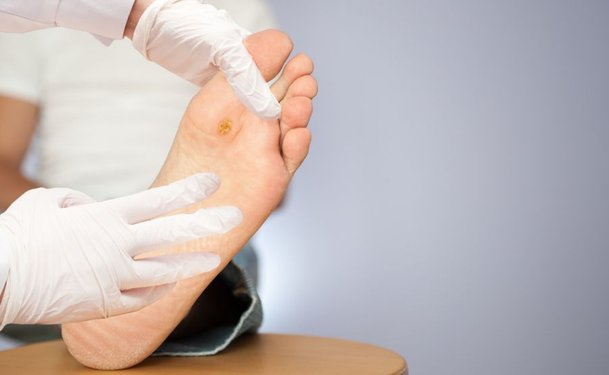
Diabetes mellitus can be virtually harmless if controlled, but the state of abnormally high blood glucose levels associated with the condition can lead to some serious complications. If left uncontrolled for a long time, or if diabetic patients fail to adapt their lifestyles in order to manage the disease, they will have more difficulty preventing complications from occurring. A serious complication that diabetics may encounter are diabetic wounds.
Causes of Diabetic Wounds
The main concern with diabetic wounds is poor or delayed healing. Healing problems are caused by the peripheral arterial diseases and peripheral neuropathy that can occur with diabetes, wherein the small blood vessels in different parts of the body, especially in the extremities (hands and feet), grow narrower and reduce the blood circulation to those areas. A lack of circulation in the extremities can result in a reduced supply of oxygen and nutrients to the body tissue and nerves, which is necessary for healing. Over time, nerves in these areas may become damaged, decreasing the sensation of pain, temperature and touch, making patients vulnerable to injury.
Types of Diabetic Wounds
For a diabetic patient, every wound is a health concern and requires immediate attention. The most common two types are wounds of external origin and wounds of internal origin. Due to peripheral neuropathy, wounds of external origin, such as skin cuts, burns, bumps and bruises, may often go unnoticed by the diabetic patient. If external wounds go unnoticed for some time, delayed treatment can put the patient at risk for further complications. Wounds of internal origin, such as skin ulcers, ingrown toenails or calluses, can lead to the breakdown of skin and surrounding tissue, increasing the risk of bacterial infections.
Signs and Symptoms of Diabetic Wounds
Diabetic wounds may present with the following signs and symptoms:
- Chronic pain or completely painless
- Signs of inflammation (swelling, redness, heat, pain and loss of function)
- Signs of infection (pus drainage, discharge, bad odor and dead tissue)
- New numbness and dullness (signs of nerve damage)
- Fever and/or chills (signs of progressively worsening infection that can be limb-threatening or even life-threatening)
Who Is at risk
Having high levels of blood glucose for extended periods makes the immune system function improperly. Due to reduced blood flow and damaged nerves, patients with uncontrolled diabetes are at high risk of developing non-healing or infected wounds. The risk is higher for diabetic patients who also have other chronic diseases, such as atherosclerosis, high cholesterol levels, obesity or AIDS. If a patient has an unhealthy diet, smokes and does not exercise, they are at greater risk for diabetic wounds. Any patient who has a hazardous occupation, such as work that involves operating heavy machinery, using sharp tools for building and construction, or violent sports, is at greater risk.
Treatment of Diabetic Wounds
The best treatment is prevention, since medical treatment for diabetic wounds provides limited help. If a wound occurs, treatment can include:
- Keeping all wounds clean and properly dressed
- Antibiotics (for infected wounds or as a preventive measure for wounds at risk of getting infected)
- Surgical debridement (the dead or infected tissue is removed to allow the healthy tissue to heal and regenerate)
- Referral to a podiatrist or a wound care center (for patients with calluses, corns, hammertoes, bunions, toenail problems or chronic non-healing ulcers)
- Limb amputation (to save as much of a limb as possible when there is a serious infection)
Prevention
Prevention of diabetic wounds is critical for diabetic patients to ensure a normal and active healthy life. It is important to remember that diabetic wounds can be disabling and life threatening in some cases. Prevention should begin with:
- Controlling diabetes by following your doctor's recommendatrions for treatment and lifestyle modifications that include a healthy diet, regular exercise, cessation of smoking and regular monitoring of blood glucose levels
- Daily inspection and cleaning of your extremities as they are more prone to ulcers and injuries
- Carefully trimming the nails with a safe nail trimmer (refer to an expert if the patient requires extra care or if there are skin lesions
- Always wear dry, clean socks to help protect your feet, and never walk barefoot (avoid tight socks that may reduce the blood circulation to the feet)